As trifling as it may seem to the layperson, aesthetic surgery is serious business. Apart from obvious cosmetic ramifications, the seriousness becomes understandable when one considers that the surgeon must first make a healthy patient temporarily unwell in order to make he or she look better in the end. It is for this very reason plastic surgeons have an added unique responsibility which surgeons of other specialties simply do not bear. Choosing to undergo elective surgery is a series of decisions made by both the surgeon and the patient. As with all aspects of medicine, nothing is absolute, it is about controlling probability.
In this day and age, patients increasingly view plastic surgery as nothing more than a haircut with a short recovery, let alone one with a complication. Even under the best of hands, a complication can arise for any number of reasons and if it does, acting as a team with your surgeon is crucial. Whether following a facelift, rhinoplasty or any plastic surgery for that matter, almost all complications can be fixed in the end, even if multiple surgical revisions are needed.
It is normal for the layman to consider surgical results as either “good” or “bad”, but those adjectives can be misleading and are certainly inadequate in revealing the true story behind the result.
“Good” surgery with a complication is not the same as “bad” surgery per se. In other words, complications do not all come from “bad” surgeons and indeed, “bad” surgeons may have successfully completed an operation without encountering obvious complications. I think it fair to say most patients consider themselves as good people and if a complication happens to them, they will perceive themselves as victims of a bad surgery and by extension, a bad surgeon. So what is the difference between “bad” surgery and a “good” surgery with a complication?
Look at it this way… in any profession, there are the “good”, the “bad” and the “excellent”. For the sake of this discussion, let’s just oversimplify the comparison between “good” and the “bad”. Since plastic surgery is as much an art (or at least an artisanal craft) as it is a science, whereby results are measured both objectively and subjectively, it is not unreasonable to compare a plastic surgeon to any artist or craftsman, including sculptors, painters and woodworkers. Artists filter their talent and vision through years of experience to not only earn but continually solidify their reputation as either being “good” or “bad”. Moreover, good artists become respected by not just producing one “good” piece but doing so consistently, whereas the “bad” consistently create sub par results as judged by the median consensus.
However, all artists, whether good or bad, are limited by the quality of material with which they work. It is known that Michelangelo’s David has been deteriorating at a far more rapid pace than would be expected because of the poor quality of its marble composition. Bernini also broke a piece of marble in half through chiseling into an unexpected vein in the stone causing him to start all over with a brand-new block. Does that make him a bad artist? Hardly not.
In other words, complications happen and that’s why there are consents to protect not only the doctor but also the patient. Consents should ensure the patients are informed as to the shared risk both they and the surgeon take when undergoing surgery.
Many complications are avoidable. Both doctors and patients must do their part to optimize a certain outcome and minimize the risk of complications. Patients must avoid certain medications that may promote bleeding, cease all smoking for optimal circulation, follow instructions and take medications as prescribed. Otherwise, surgery may be self-sabotaged. On the other hand, surgeons must do their part in educating and performing the proper operation in the right patient with skill and dedication.
Other complications are unavoidable and just because they may be explainable in hindsight does not mean they were avoidable within the context they occurred. This is why it is paramount that patients disclose all of their medical history and follow their surgeon’s instructions to a T in order to minimize unexpected situations such as abnormal bleeding, poor wound healing, etc..
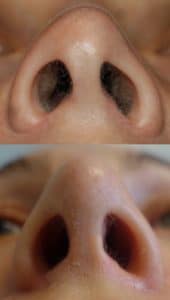
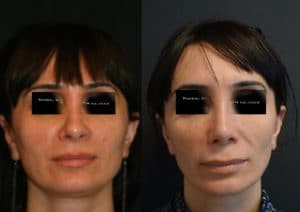
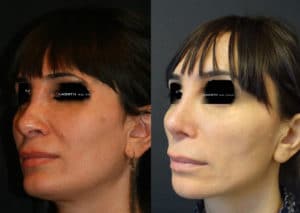
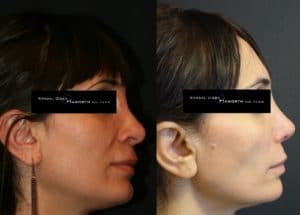
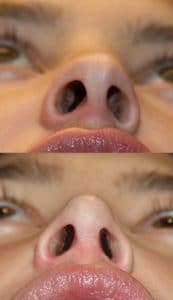
What spurred me to write this particular blog was a recent experience having performed a complex revision rhinoplasty on a dear friend of mine of 20 years. Unfortunately, this advanced detailed nasal reconstruction was exacerbated by unexpected physiological conditions including excessive bleeding and poor tissue characteristics. The next day, the patient presented with so much swelling underneath the pressure cast that it was being pushed off the face. The swelling was a hematoma which I immediately evacuated from under the skin (it was 4 1/2 mL, being the largest nasal hematoma encountered by either my colleagues or myself). Accompanying this was necrosis (death) of the columellar skin (the partition separating his left and right nostrils). This was particularly disappointing to say the least because the surgical results in terms of nasal shape, symmetry, tip definition and projection were otherwise excellent. Yet losing coverage over the columella would have serious ramifications.
Despite attempts to bring vascularized tissue using local intraoral flaps, my friend eventually needed the help of a certain specialist to bring fresh tissue to the columella below the nasal tip with a temporary forehead flap.
Albeit exceedingly rare, this 1.5 x 1.2 cm skin loss was enough to eradicate not only their trust in me as a surgeon but also our long term friendship. Most patients understandably experience a spectrum of emotions including panic, sadness, denial, anger and ultimately acceptance from a complication such as this. However, nothing could prepare me for the degree of ongoing vengeful anger and hostility the patient and their partner have directed towards me including threats to go to the press and ruin my reputation.
Anger is not only destructive but also lacks focus, therefore it can be especially counterproductive to both healing and a good result (not to mention friendship!). Premature castigations of blame fuel brash, illogical decisions which actually complicate the original complication.
Understanding the differences between “bad” and “good” surgery and “good” surgery with a complication can certainly help put things in perspective. When a patient concedes the net surgical aesthetic result, at least in terms of shape and symmetry, as good if not excellent, he or she is less likely to question, and more likely trust, their original choice of surgeon. Whether their breast lift incision opened or, as in this case, a small but strategic portion of nasal skin died, the affected patient will see the “bigger picture” and believe their surgeon will do the right thing by having their best interests at heart. This same patient understands that they were not necessarily a victim or unjustifiably punished by “bad” surgery. Instead, they will accept things for what they are, learn patience and develop a sense of optimism to set themselves up for the best possible outcome in the future.
The majority of complications concern wound healing and minor infections. For these, possible antibiotics and the “tincture of time” for healing to occur are required. Other times, simple, clinical interventions such as laser treatment, injections, the occasional scar revision and creams are all that are needed.
Other complications require more invasive solutions. Depending on the type of complication, an expeditious trip to the operatory maybe all that is required (e.g.,to drain a hematoma) whereas staged surgical revisions may be undertaken in the extremely rare case of tissue loss.
Most surgeons will recognize if a particular complication is beyond their level of expertise. A patient should not feel abandoned or simply passed off if they are referred to another expert if a complication warrants it. It is important to recognize that medicine is team work and the referral is simply a reflection of the original surgeon’s dedication to the best outcome possible.
Emotional advice after a complication
–Watch out for advice with an agenda. It is understandable that if a complication does arise, fear and anxiety will prompt you to seek solace and advice from friends and family members. While this is wholeheartedly encouraged, it is important to remember that not all the advice given is good especially considering that those giving advice are not often doctors nor do they know the intricate details of the patient’s particular case. Though most advice is well-meaning in intent, some may be motivated by guilt, jealousy, personality disorders or just plain ignorance. Furthermore, the advice a patient may obtain from elsewhere may be counterproductive because it may only increase their level of anxiety.
–Stay optimistic and avoid jumping to any pessimistic conclusions. It is not unheard of that acute anxiety will provoke a patient to impatiently reach for the help of an alternative plastic surgeon. Unfortunately, some plastic surgeons may be unscrupulous and advise the fragile, highly suggestible patient into unnecessary and ill-timed surgery claiming it is urgently needed to prevent some permanent deformity. Always keep a line of communication open with the original plastic surgeon to not only help allay personal fears but also be guided in the right direction with a second opinion if necessary.
“A good patient is an educated patient”-
Randal D. Haworth M.D., F.A.C.S.
Board Certified Plastic Surgeon
Beverly Hills